Serviços Personalizados
Journal
Artigo
Compartilhar
Revista Brasileira de Educação Médica
versão impressa ISSN 0100-5502versão On-line ISSN 1981-5271
Rev. Bras. Educ. Med. vol.49 no.2 Rio de Janeiro 2025 Epub 15-Maio-2025
https://doi.org/10.1590/1981-5271v49.1-2023-0057
REVIEW ARTICLE
Teaching funduscopy to undergraduate medical students: trends in the literature
1 Universidade do Estados do Pará, Marabá, Pará, Brazil.
2 Universidade do Estado do Pará, Belém, Pará, Brazil.
Introduction:
Funduscopy is a skill that should be utilized by medical professionals, especially in clinical contexts associated with systemic arterial hypertension (SAH), diabetes mellitus (DM) and neurological conditions. The teaching of this topic in medical undergraduate courses is a recurring subject in the literature, including approaches that consider not only the teaching of direct ophthalmoscopy (DO) but also techniques based on obtaining and analyzing images of the fundus.
Objective:
To identify and analyze experiences and trends in the literature on the teaching of funduscopy in medical undergraduate courses.
Results:
A total of 44 articles were selected through the review. The use of simulators and fundus images captured with devices coupled to cell phone cameras were teaching resources used in a large number of studies (52.3% of articles) with positive conclusions about the use of these elements for learning funduscopy. Direct ophthalmoscopy continues to be a recommended technique, although most studies identify difficulties in its learning and performance. Most research used controlled environments, had little follow-up time to ascertain the efficiency of the teaching processes and lacked uniform and clear educational objectives and learning methodologies that should be used in teaching funduscopy. Only two studies were carried out in authentic care environments.
Conclusion:
There are several experiences reported on the teaching of funduscopy supported by various resources that proved to be pedagogically appropriate. Longitudinal and methodologically uniform studies must be conducted to obtain reproducible and comparable results that can warrant better efficiency in the teaching of funduscopy in medical education.
Keywords: Medical Education; Ophthalmoscopy; Teaching; Fundus oculi
Introdução:
O exame de fundo de olho (EFO) é um recurso semiológico importante e deve ser uma competência exercida pelo profissional médico, especialmente em contextos clínicos associados a hipertensão arterial sistêmica (HAS), diabetes mellitus (DM) e quadros neurológicos. O ensino do EFO na graduação médica é um tema recorrente e desafiador na literatura com experiências que consideram não somente o ensino da oftalmoscopia direta (OD), mas também técnicas de exame que se baseiam na obtenção e análise de imagens do fundo de olho.
Objetivo:
Este estudo teve como objetivos identificar e analisar na literatura experiências e tendências sobre o ensino do EFO na graduação médica.
Método:
Trata-se de uma pesquisa descritiva literária que coletou publicações compreendidas no período de 2013 a 2023.
Resultado:
Foram selecionados 44 estudos publicados no período. O uso de simuladores e de imagens obtidas com dispositivos acoplados a câmeras de telefones celulares apresentou-se em 52,3% dos estudos com conclusões positivas sobre a utilização desses elementos para a aprendizagem do EFO. A OD continua sendo uma técnica recomendada e ensinada, muito embora a maioria dos estudos identifique dificuldades em seu aprendizado e exercício. A maioria das pesquisas utilizou ambientes controlados, teve pouco tempo de seguimento no sentido de averiguar a eficiência dos processos de ensino testados e não definiu com clareza os objetivos educacionais e as metodologias de aprendizagem que devem ser empregados no ensino do EFO. Somente dois estudos foram conduzidos em ambientes autênticos de atendimento.
Conclusão:
Existem várias experiências relatadas sobre o ensino do EFO amparadas por diversos recursos que se mostraram pedagogicamente adequados. Estudos longitudinais e metodologicamente uniformes devem ser conduzidos para a obtenção de resultados reprodutíveis e comparáveis que possam garantir eficiência ao ensino do EFO na graduação médica.
Palavras-chave: Educação Médica; Oftalmoscopia; Ensino; Fundo de Olho
INTRODUCTION
The literature on the teaching of fundoscopy in undergraduate medical courses is in agreement in the sense that medical students should recognize the importance of this semiological procedure and know how to proceed to access and analyze the fundus, especially in clinical contexts - many of them critical - related to systemic arterial hypertension (SAH), diabetes mellitus (DM) and neurological conditions1),(2),(3. A study carried out in the state of Pará concluded that 58.7% of a sample of patients treated at a primary health care unit with SAH and/or DM and examined by direct ophthalmoscopy (DO) had fundus abnormalities4.
Teaching-learning and the practice of the traditional DO technique for fundoscopy have limitations. Studies conducted with students and physicians who have already graduated have shown that the vast majority do not satisfactorily perform direct ophthalmoscopy5),(6),(7),(8. There are controversies in the literature about this examination technique, with opinions that question its efficiency and question the validity of its teaching. However, most authors defend their learning, even recognizing their limitations9),(10),(11.
Direct ophthalmoscopy requires skills that can only be improved with constant training and performance. It is recognized the fact that during undergraduate studies there is little availability for the teaching and practicing of this competency12. A recent study conducted in the state of Mato Grosso (Brazil) showed that only about 10% of the medical students interviewed in the survey considered themselves to master the practice and theory related to direct ophthalmoscopy13. This reality, together with other factors, such as the need for mydriasis and adequate environments for the examination, the influence of media opacity, and the small observable field, contributes to making both the learning and the practice of direct ophthalmoscopy challenging14),(15),(16.
In this context, studies have addressed several possibilities for teaching fundoscopy, many of them using simulators, in addition to testing other evaluation techniques, especially by obtaining and analyzing photographs of the posterior ocular pole, which is currently possible with the use of portable devices that, in general, work coupled to cell phone cameras17),(18),(19. Biousse et al.20 defend the acquisition of fundus images, stating that “effectively visualizing the fundus is more important than (discussing) the technique used for this purpose”.
In view of the need to teach fundoscopy in clinically relevant situations from an epidemiological point of view, it is important to address the problem of its performance and learning to ensure adequate training of general practitioners in accordance with the National Curriculum Guidelines for medical education. This review aims to explore pedagogical experiences that indicate solutions for the optimization of the approach to this topic in medical courses.
OBJECTIVE
To describe and analyze the experiences and trends that are found in the scientific literature on the fundus examination, aiming to improve the teaching of fundoscopy in medical undergraduate courses.
METHOD
This is a literature review based on the following guiding question: “What are the examination techniques and teaching strategies that have been evaluated for the teaching of fundoscopy among medical students?”.
During data collection, a search was conducted for articles published in the last ten years (01/01/2013 - 07/06/2023), without language restrictions and using the following databases: Scielo; Virtual Health Library (VHL); PubMed; Cochrane; Web of Science; Capes Periodicals; Embase. Keywords were defined to set up the search strategies,. The main keywords searched were: (“Exame de fundo de olho” or “Fundoscopia” or “Oftalmoscopia direta”) or (“Direct ophthalmoscopy” or “Fundoscopy”) and (“Ensino” or “Teaching” or “Enseñanza” or “Enseignement”) and (“Direct ophthalmoscopy” or “Fundoscopy” or “Fundus examination”) and (“Teaching” or “Technics, Training” or “Training Technics”).
The inclusion criteria included fully published articles that reported experiences in teaching the fundus exam, whereas abstracts in conference proceedings, articles with incomplete text, letters to editors, and publications of preliminary results were excluded. Review articles or articles on the teaching of fundoscopy in post-graduation were excluded.
The material obtained in the search was exported to a folder of the Rayyan ® program, and duplicates were excluded. The articles were initially evaluated by reading titles and abstracts in relation to the inclusion and exclusion criteria and the search topic. Studies cited by the bibliographic references were also identified. The selected publications (44 articles) were read in full by the researchers, and analysis guides were filled out with the following items, which were cataloged in a Microsoft Excel 365® file: bibliometric data (main author, medical specialty, institution and country to which the main author is linked, journal of publication), general study design, main objective, sample characteristics and methodology and summary of conclusions.
RESULTS
Listed articles
As shown in the flowchart (Figure 1), 691 studies were initially identified, of which 265 duplicates were excluded. The titles and abstracts of the 426 articles were read and analyzed, and 378 articles were excluded because they were not publications whose topic was in fact the teaching of the fundus examination aimed at medical students (these were articles of studies or various issues related to ophthalmoscopy or teaching at other levels of medical education, such as a residency). Thus, 48 studies were selected for reading in full. At the end of this process, eight more articles were excluded (4 abstracts, 2 letters to editors, and 2 that were not related to the undergraduate level) and 4 publications selected through search in the references were included. Thus, the final sample consisted of 44 publications, which comprise this review.
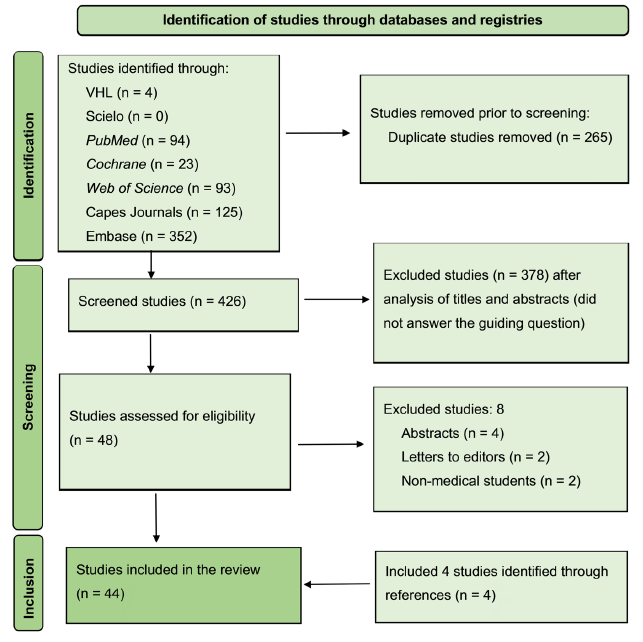
Source: prepared by the authors, 2024.
Figure 1 Flowchart on article collection for bibliographic review.
All 44 articles report experiences of teaching fundoscopy in undergraduate medical studies conducted in controlled research settings or in real care settings. As teaching strategies, the publications refer to the use of simulators, the capture of fundus images with equipment coupled to cell phone cameras, direct peer ophthalmoscopy training and several other resources. Regarding the type of evaluation of educational interventions, the studies describe summative and formative evaluation processes that generated data used for analysis and measurement of the intervention results, which included (but not in all experiences) the comparison between different study groups or between these and control groups, the latter generally consisting of training with a direct ophthalmoscope without the aid of other complementary resources.
Charts 1, 2 and 3 list the main author, the main educational institution linked to the study, the country in which the research was conducted and the year of publication of the article.
DISCUSSION
The main objective of this research was to study the scientific literature on fundoscopy aiming to improve the teaching of the subject in undergraduate medical courses. In order to simplify the analysis and discussion of the results, the articles were categorized into three major groups (Graph 1):
Group 1 − Experiments with the use of fundus simulators;
Group 2 − Experiences with the use of fundus photographs obtained with devices attached to cell phone cameras (smartphones);
Group 3 − Experiences of teaching fundoscopy with several resources.
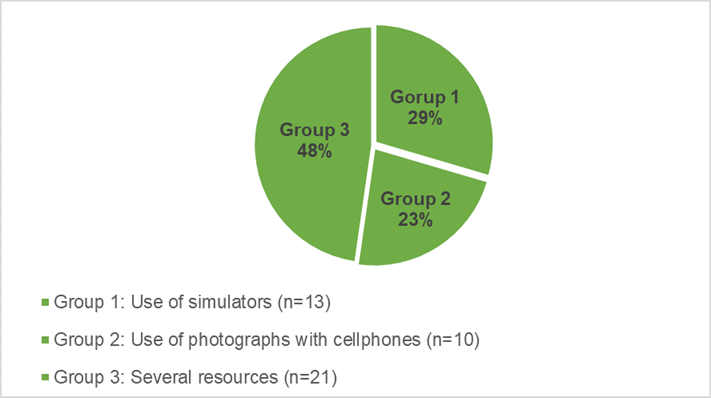
Graph 1 Distribution of the reviewed articles by group according to the didactic resources used for teaching fundoscopy:
Next, the findings related to the set of each of the abovementioned groups will be presented and discussed.
Analysis and discussion of the articles of group 1: experiences with the use of fundus simulators
As summarized in chart 1, of the total number of retrieved articles, 13 studies focused on the use of simulators (29.5% of the studies).
Chart 1 Articles listed for bibliographic review on the teaching of fundoscopy. GROUP 1 - Use of fundus simulators for the teaching of fundoscopy.
| ARTICLE | AUTHOR | RESEARCH INSTITUTION | COUNTRY | YEAR |
|---|---|---|---|---|
| 1 | Kelly et al.2 | Emory University | USA | 2013 |
| 2 | Akaishi et al.21 | Tokyo Medical University | Japan | 2014 |
| 3 | Wu et al.22 | Northwestern University | USA | 2014 |
| 4 | Larsen et al.23 | University of Nebraska | USA | 2014 |
| 5 | Androwiki et al.24 | Universidade Federal de São Paulo | Brasil | 2015 |
| 6 | Yusuf et al.25 | Oxford Medical School | United Kingdom | 2016 |
| 7 | Martins et al.12 | Universidade Federal de São Paulo | Brazil | 2017 |
| 8 | Souza et al.26 | Universidade Federal do Piauí | Brazil | 2017 |
| 9 | Deuchler et al.27 | Goethe-Universität Frankfurt am Main | Germany | 2022 |
| 10 | Mahmoud et al.28 | Université de Monastir | Tunisia | 2021 |
| 11 | Tso et al.29 | Indiana University School of Medicine | USA | 2021 |
| 12 | Wu et al.30 | Pekin Union Medical College | China | 2022 |
| 13 | Howell et al.31 | Ucla Stein Eye Institute | USA | 2021 |
Source: prepared by the authors, 2024.
For the purposes of discussion, two types of simulators stand out in the studies selected in this review: simulators sold commercially at high cost and low-cost simulators, usually manufactured and designed by the authors themselves.
Among the highest cost simulators, the following products were identified: EYE Simulator (Kyoto Kagaku), Eyesi Direct (VRmagic) and Eye Retinopathy Trainer (Adam, Rouilly).
Akaishi et al. (2014)21 and Larsen et al. (2014)23 investigated the EYE Examination Simulator as a teaching tool for medical students, with samples, respectively, of 90 and 115 students. They concluded that the use of the simulator in the study group allowed a greater number of correct answers in assessment tests and greater confidence in the examination performance, as it allowed an increase in the frequency of fundoscopy training. In the same sense of positive evaluation regarding the use of simulators, one can mention the studies conducted by Tso et al. (2021)29 and Deuchler et al. (2021)27, in which the Eyesi Direct (VRmagic) equipment was used as a teaching tool. Favorable conclusions to the use of simulators were also presented in three independent studies, conducted by Androwiki et al. (2015)24, Mahmoud et al. (2021)28 and Yusuf et al. (2017)25, who analyzed the Eye Retinopathy Trainer (Adam, Rouilly). The intentional samples of these studies were, respectively, 90, 160 and 48 students and the results indicated that the simulator use allowed the improvement of the skills and knowledge necessary to perform the fundoscopy.
Analysis and discussion of the articles of group 2: experiences with the use of fundus photographs obtained with devices attached to cell phone cameras (smartphones)
In the study by Wu et al. (2014)22, which involved a small sample of 12 students and evaluated the performance of a simulator called FAK-I, the results indicated that the group of students who used the tool obtained a slightly higher percentage of correct answers in the evaluation process than the control group, but without a statistically significant result.
A study conducted by Souza et al. (2017)26, with the participation of 24 students, analyzed the performance of two distinct groups. In the group that used a simulator, the objective mean score in the evaluation process was considerably higher, reaching 82%, compared to the group that underwent training with human volunteers, which obtained a mean score of 45% (p = 0.01). These results indicate a statistically significant difference favoring the group that used the simulator, suggesting that it was effective in teaching fundoscopy. It is noteworthy that there was no statistically significant difference between the groups in relation to the degree of difficulty experienced in performing the exam.
Martins et al. (2017)12 developed an educational model that involves the construction of an artisanal simulator . This instrument consists of a transparent acrylic sphere with a radius of 1.1 cm, inserted in a cardboard box, with openings that represent the pupils. Inside the model, 1 cm × 1 cm images containing words, numbers and images of the ocular fundus were inserted. The total cost of the material was about US$ 1.00 or R$ 5.00. This practice also helped to illustrate the concepts of physics pertinent to fundoscopy, making the learning process more engaging.
In the study conducted by Howell et al. (2022)31, with the participation of 33 students, the main objective was to analyze the effects of frequent practice in simulators. Those who practiced more regularly showed improvements. Moreover, an increase in the ability to identify fundus lesions was observed, a core competence in fundoscopy. These results suggest that regular practice plays an important role in improving skills for the performance of fundoscopy. Similar results were described by Wu et al.30 in an experiment that involved a sample of 92 students.
Overall, the use of several simulator models showed a positive impact on medical students’ learning, although none of the studies were longitudinal and, therefore, not able to measure the results in terms of knowledge retention or performance improvement in the long term. Many of the studies involved small sample sizes, which reduces confidence in the level of evidence generated by these studies.
It should be noted that performing direct ophthalmoscopy in real-life environments of care, peer training or with volunteer patients is not able to obtain samples of the various pathological signs of the fundus that are found in specific and infrequent situations, such as, for example, papilledema and subretinal hemorrhage, which may be present in intracranial hypertension and in patients with subarachnoid hemorrhage, among others. Thus, in addition to allowing constant repetition in the training of procedures, one of the advantages of using simulators is the fact that it also provides the observation of infrequent fundus changes in authentic environments. It is important to emphasize that the positive value of clinical and surgical simulations has long been recognized as effective complementary strategies that increase the level of safety in health professionals’ training32),(33),(34),(35),(36.
Chart 2 Articles listed for the review of the teaching of fundoscopy. Group 2 − Use of fundus photographs obtained with devices attached to cell phone cameras.
| ARTICLE | AUTHOR | INSTITUTION | COUNTRY | YEAR |
|---|---|---|---|---|
| 14 | Mantora et al.37 | Sunderland Eye Infirmary | United Kingdom | 2018 |
| 15 | Wu et al.38 | University of Nebraska Medical Center | USA | 2018 |
| 16 | Kim et al.39 | University of California | USA | 2019 |
| 17 | Shikino et al.40 | Chiba University School of Medicine | Japan | 2019 |
| 18 | Wang et al.41 | Shantou University | China | 2023 |
| 19 | Curtis et al.42 | Kingston General Hospital | Canada | 2021 |
| 20 | Franzco et al.43 | University of Sydney | Australia | 2021 |
| 21 | Kohler et al.44 | University of Minnesota | USA | 2021 |
| 22 | Ahmed et al.45 | University of Toronto | Canada | 2022 |
| 23 | Qader et al.46 | University Joint-Committee | Malaysia | 2022 |
Source: prepared by the authors, 2024.
Of the total of 44 articles, ten articles were identified that studied the use of fundus photographs obtained with smartphones (22.7% of the retrieved articles). The years of publication were concentrated in the period from 2018 to 2023, showing that this teaching strategy and fundus assessment technique is depicted in relatively recent experiences, although the use of non-mydriatic cameras for fundus photography in various scenarios has been the subject of study for years17),(18. A recent study carried out in São Paulo, Brazil, on the use of cell phone cameras used to detect diabetic retinopathy with the support of telediagnosis presented interesting results for the screening of this condition in primary health care47.
In principle, it should be noted that one of the great advantages of the photographic record of the fundus concerns the possibility of filing, editing and sharing the photograph remotely, allowing remote evaluation (telediagnosis) and a more detailed analysis of the ocular structures. Fundus photographs obtained with portable devices in authentic care environments have already been the subject of competent studies that reinforce this technique usefulness, even suggesting its superiority in terms of accuracy over direct ophthalmoscopy48.
The main devices integrated into smartphone cameras were the D-EYE device (Italy) and the iExaminer (Welch Allyn, Australia), the first of which was directly coupled to a smartphone, whereas the second also required a Panoptik direct ophthalmoscope (Welch Allyn, Australia).
Studies conducted by Wu et al. (2018)38, Curtis et al. (2021)42 and Franzko et al. (2021)43) demonstrated that capturing fundus photographs with the D EYE device can facilitate the learning of fundoscopy by medical students. It should be noted, however, that these studies did not have sufficient follow-up time to assess the real long-term impacts on learning. Coincident results were reported by Shikino et al. (2019)40) who tested the use of the iExaminer in a sample of 115 students in a study in which they associated the use of the EYE Examination Simulator (Kyoko Kagaku Co) and concluded that the learning method with these elements improved the accuracy and overall performance of students when performing the fundoscopy.
In the same sense, Kim et al. (2019)39, in a study with a sample of 101 medical students, also identified a preference for fundus photographs and better student performance when using this technique. As weaknesses in this study, it should be mentioned that the structure evaluated was limited to the optic disc − similarly to other studies in this selection −, and the ophthalmoscopy was performed in non-dilated pupils, which does not correspond to the examination technique, which should preferably be performed in mydriasis. The statistical differences in the evaluation of the students’ performance (control and intervention groups) were not high, suggesting that the use of photographs can be useful in learning, but does not disallow the teaching and evaluation of the fundus through traditional direct ophthalmoscopy.
Analysis and discussion of the articles of group 3: diverse experiences of teaching fundoscopy
Chart 3 Articles listed for review on the teaching of fundoscopy. Group 3 - Diverse teaching experiences.
| ARTICLE | AUTHOR | INSTITUTION | COUNTRY | YEAR |
| 24 | Milani et al.49 | University of Illinois | USA | 2013 |
| 25 | Krohn et al.50 | University of Minnesota | Norway | 2014 |
| 26 | Byrd et al.51 | University of New Mexico | USA | 2014 |
| 27 | Lowe et al.52 | Eastbourne District General Hospital | United Kingdom | 2015 |
| 28 | Schulz et al.53 | Brighton and Sussex School | United Kingdom | 2016 |
| 29 | Lippa et al.54 | University of California | USA | 2015 |
| 30 | Yusuf et al.55 | Oxford Eye Hospital | United Kingdom | 2016 |
| 31 | Kwok et al.56 | Queen’s University | Canada | 2017 |
| 32 | Wilson et al.57 | Birmingham City University | United Kingdom | 2017 |
| 33 | Bénard S et al.58 | University of Calgary | Canada | 2017 |
| 34 | Gilmour et al.59 | Michigan State University | USA | 2017 |
| 35 | Dissanayake et al.60 | University of Colombo | Sri Lanka | 2017 |
| 36 | Boden et al.61 | Saarland University Med Center | Germany | 2019 |
| 37 | Gilmour-W et al.62 | Birmingham City University | United Kingdom | 2019 |
| 38 | Lee et al.63 | University of Miami | USA | 2020 |
| 39 | Rose et al.64 | Christian Medical College | India | 2021 |
| 40 | Ayub et al.7 | Universidade de Campinas | Brazil | 2021 |
| 41 | Dunn et al.65 | University of Sydney | Australia | 2021 |
| 42 | Shikino et al. (66) | Chiba University Hospital | Japan | 2021 |
| 43 | Vloka et al. (67) | University of Pittsburgh | USA | 2022 |
| 44 | Henick et al. (68) | Icahn School of Medicine | USA | 2020 |
Source: prepared by the authors, 2024.
In this category, 21 articles were collected (47.8% of the total number of articles listed in this review).
The use of fundus photographs as a support in learning dynamics was identified in studies conducted by Milani et al. (2013)49, Krohn et al. (2014)50, Bénard-Séguin et al. (2017)58, Kwok et al. (2017)56 and Gilmour et al. (2017)59, demonstrating that these resources are widely used in several teaching strategies.
Real-life scenarios were reported in only two articles. One of them by Yusuf et al. (2016) in a teaching experience in a primary health care service; the other by Byrd et al. (2014)51, who report a health action with vulnerable populations in New Mexico, and one quality of this last experience is the verification of skill retention after one year of integrated teaching and care activities.
Other studies have used diversified strategies, such as audiovisual resources such as videotapes to demonstrate the exam technique (Dissanayake et al., 2017)60, a virtual teaching environment developed in the southern region of India during the Covid-19 epidemic (Rose et al., 2020)64, peer-training (Henick et al., 2017) (68) , virtual and multisensory teaching model (Lippa et al., 2015)54, among others.
Ayub et al. (2021)7, in a recent study conducted with medical students at the University of Campinas (Unicamp, Brazil), represent one of the few longitudinal studies in this review, evaluating skill retention over a one-year period, comparing the Panoptik ophthalmoscope (Welch Allyn) and the traditional coaxial ophthalmoscope (Welch Allyn). The sample comprising 167 students is another positive aspect of this study, which indicates the same difficulties, according to other publications already documented, to maintain, in the long term, the skills and knowledge necessary for the competent performance of fundoscopy.
A study conducted by Gilmour-White et al. (2019)57 identified that, even with easy access to direct ophthalmoscopes, students did not maintain the habit of performing or maintaining confidence in the exam. Schulz et al. (2015)48, identifying that one of the difficulties in learning the direct ophthalmoscopy technique was the impossibility of sharing the observation of the fundus with an instructor, developed an ophthalmoscope model that allows the instructor to observe the fundus together with the examiner/student. Although it is desirable and valuable, this innovation does not seem to have become widely used.
Finally, the study called Efocus 1, conducted by Dunn et al. (2021)60 in a sample of 146 second-year medical students, identified the students’ good perception regarding methods with image recording in criteria such as usability and easy to perform in relation to other fundus assessment techniques, corroborating the students’ good response to obtaining and analyzing fundus photographs, a phenomenon also identified in other studies such as those conducted by Curtis et al. (2021)42 and Franzko et al. (2021)43) .
FINAL CONSIDERATIONS
Fundoscopy remains a challenging topic in medical education. The literature indicates that the direct ophthalmoscopy practice and the acquisition and interpretation of fundus images should and can be competencies of the medical professional. As reported, an important group of educational interventions describes the use of simulators, indicating simulation techniques as possible and effective in the teaching-learning process of ophthalmoscopy. Fundus photographs obtained with portable devices were cited in several analyzed studies and the conclusions were also favorable regarding the use of these resources. Thus, it is suggested that the use of these devices be incorporated into the teaching processes of fundoscopy in medical education institutions.
Training in real-life care environments constituted the absolute minority of the studies, demonstrating that the practice of fundoscopy does not seem to be stimulated and incorporated into medical students’ daily lives. Almost all of the 44 studies included in this review were, symptomatically and paradoxically, conducted by ophthalmologists, with very little participation from other specialties. Other studies on fundoscopy in general have occurred at levels of medical specialization, with publications mainly in the areas of neurology and pediatrics. A gap is identified due to the fact that the studies do not seek to clearly and rigorously identify what would be the objectives of learning fundoscopy in medical undergraduate courses, and even less how the teaching and performance of this competence should be stimulated, reviewed and evaluated throughout the undergraduate course in the context of integrated medical curricula.
This review, considering the analytical limitations of narrative studies, summarizes a series of teaching modalities, strategies, and resources with the potential to have a positive impact on the teaching of fundoscopy in medical undergraduate studies. The judicious use of these resources in a longitudinal teaching plan anchored in the concepts of an integrated curriculum and meaningful learning, with interventions that take advantage of opportunities and scenarios throughout the medical course and that are clear in the definition of educational objectives and evaluation processes, can be a way to improve and ensure efficiency in the teaching of fundoscopy.
REFERENCES
1. Benbassat J, Polak BCP, Javitt JC. Objectives of teaching direct ophthalmoscopy to medical students. Acta Ophthalmol. 2011;90(6):503-7. doi: https://doi.org/10.1111/j.1755-3768.2011.02221.x. [ Links ]
2. Kelly LP, Garza PS, Bruce BB , ,Graubart EB, Neuman NJ, Biousse V Teaching ophthalmoscopy to medical students (the TOTeMS study). Am J Ophthalmol. 2013;16(5):1056-61. doi: http://dx.doi.org/10.1016/j.ajo.2013.06.022. [ Links ]
3. Wang H, Liao X, Pang CP, Chen H. Smartphone ophthalmoscope as a tool in teaching direct ophthalmoscopy: a crossover randomized controlled trial. Med Educ Online. 2023;28(1):1-9. doi: http://dx.doi.org/10.1080/10872981.2023.2176201. [ Links ]
4. Alves AP, dos Santos RNV, Sobrinho EFA, Rocha SP, Lock SC. Retinopatia em pacientes hipertensos e/ou diabéticos em uma unidade de saúde da família. Rev Bras Oftalmol 2014;73(2):108-11. doi: http://dx.doi.org/10.5935/0034-7280.20140024. [ Links ]
5. Gilmour G, Mckivigan J. Evaluating medical students’ proficiency with a handheld ophthalmoscope: a pilot study. Adv Med Educ Pract. 2016;2(8):33-6. doi: https://doi.org/10.2147/AMEP.S119440. [ Links ]
6. Gupta RR, Lam Wai-Ching. Medical students’ self confidence in performing direct ophthalmoscopy in clinical training. Can J Ophthalmol. 2006;41(2):169-74. doi: https://doi.org/10.1139/I06-004. [ Links ]
7. Ayub G, Souza RF, Albuquerque AM, Vasconcelos JPC. Comparison of conventional and wide field direct ophthalmoscopy on medical students’ self-confidence for fundus examination: a 1-year follow-up. BMC Med Educ. 2021; 21(1):507-13. doi: https://doi.org/10.1186/s12909-021-02942-y. [ Links ]
8. Kahwage SG, Braga TKK, Portela MV, Andriolo RB. O ensino de habilidades clínicas e a aplicabilidade de um guia simplificado de exame físico na graduação de medicina. Rev Bras Educ Med. 2017;41(2):299-309. doi: https://doi.org/10.1590/1981-52712015v41n2RB20160110. [ Links ]
9. Purbrick RMJ, Chong NV. Direct ophthalmoscopy should be taught to undergraduate medical students - no. Eye (Lond). 2015; 29(8):990-1. doi: https://doi.org/10.1038/eye.2015.91. [ Links ]
10. Yusuf IH, Salmon JF, Patel CK. Direct ophthalmoscopy should be taught to undergraduate medical students - yes. Eye. 2015;29(3):987-9. [ Links ]
11. Orlans HO. Direct ophthalmoscopy should be taught within the context of its limitations - no. Eye (Lond) . 2016; 30(2):326-7. doi: https://doi.org/10.1038/eye.2015.225. [ Links ]
12. Martins TG, Costa ALF, Helene O, Martins RV, Helene AF, Schor P. raining of direct ophthalmoscopy using models. Clin Teac. 2017 Dec; 14(6):423-6. doi: https://doi.org/10.1111/tct.12641. [ Links ]
13. Esidio AV, Angeloni CRM. Análise do ensino da oftalmoscopia direta nos cursos de graduação de Medicina do Estado do Mato Grosso. Rev Bras Oftalmol . 2020;79(1):21-7. doi: https://doi.org/10.5935/0034-7280.20200076. [ Links ]
14. Mamtora S, Sandinha MT, Ajith A, Song A, Stew DHW. Smartphone ophthalmoscopy: a potential replacement for the direct ophthalmoscope. Eye (Lond) . 2018;32(11):1766-71. doi: https://doi.org/10.1038/s41433-018-0177-1 [ Links ]
15. Dunn HP, Marks S, Teo KZ, Dunn SM, Healey PR, White AJ. eFOCUS 2: A randomised crossover trial of smartphone fundoscopy and direct ophthalmoscopy aiming to improve optic disc interpretation by medical students with e-learning support. Clin Exp Ophthalmol. 2021;49(7):704-13. doi: https://doi.org/10.1111/ceo.13977. [ Links ]
16. Milani LZ, Pich S, Edelweiss MK. Barreiras para a realização de oftalmoscopia direta por médicos de família e comunidade. Rev Bras Med Fam Comunidade. 2022;17(44): 2970-5. doi: https://doi.org/10.5712/rbmfc17(44)2970. [ Links ]
17. Bruce BB, Biousse V, Newmann NJ. Nonmydriatic ocular fundus photography in neurologic. JAMA Neurol. 2015;72(4):455-9. doi: https://doi.org/10.1001/jamaneurol.2014.4053. [ Links ]
18. Mackay DD, Bruce BB Non-mydriatic fundus photography: a practical review for the neurologist. Pract Neurol. 2016;16(5):343-51. doi: https://doi.org/10.1136/practneurol-2016-001443. [ Links ]
19. Ricci LH, Ferraz CA. Ophthalmoscopy simulation: advances in training and practice from medical students and young ophthalmologists. Advances in Medical Education and Practice 2017;8:435-9. doi: https://doi.org/10.2147/AMEP.S108041. [ Links ]
20. Biousse V, Bruce BB, Newman NJ.Ophthalmoscopy in the 21 st century: the 2017 H Houston Merrit Lecture. Neurology.2018;90(4):167-75.doi: https://doi.org/10.1212/WNL.0000000000004868. [ Links ]
21. Akaishi Y, Otaki J, Takahashi O, Breugelmans R, Kojima K, Seki M, et al. Validity of direct ophthalmoscopy skill evaluation with ocular fundus examination simulators. Can J Ophthalmol . 2014 Aug;49(4):377-81. doi: http://dx.doi.org/10.1016/j.jcjo.2014.06.001. [ Links ]
22. Wu G, Kang J, Bidwell A, Gray J, Mirza R. The use and evaluation of an inexpensive eye model in direct ophthalmoscopy training. J Acad Ophthalmol. 2014 Dec 23;07(01):21-5. doi: http://dx.doi.org/10.1055/s-0034-1396412. [ Links ]
23. Larsen P, Stoddart H, Griess M. Ophthalmoscopy using an eye simulator model. Clin Teach. 2014 Mar 14;11(2):99-103. doi: http://dx.doi.org/10.1111/tct.12064. [ Links ]
24. Androwiki JE, Scravoni IA, Ricci LH, Fagundes DJ, Ferraz CA. Evaluation of a simulation tool in ophthalmology: application in teaching funduscopy. Arq Bras Oftalmol. 2015;78(1).36-9 doi: http://dx.doi.org/10.5935/0004-2749.20150010. [ Links ]
25. Yusuf IH, Ridyard E, Fung THM, Sipkova Z, Patel CK. Integrating retinal simulation with a peer-assessed group OSCE format to teach direct ophthalmoscopy. Can J Ophthalmol . 2017 Aug;52(4):392-7. doi: http://dx.doi.org/10.1016/j.jcjo.2016.11.027. [ Links ]
26. Souza PHL de, Nunes GMN, Bastos JMG de A, Fonseca TM, Cortizo V. A new model for teaching opthalmoscopy to medical students. MedEdPublish. 2017 Nov 6;6:197.1-15 doi: http://dx.doi.org/10.15694/mep.2017.000197. [ Links ]
27. Deuchler S, Sebode C, Ackermann H, Schmack I, Singh P, Kohnen T, et al. Kombination von simulationsbasiertem Lernen und Online-Learning in der Augenheilkunde. Der Ophthalmologe. 2021;119(1):20-9. doi: http://dx.doi.org/10.1007/s00347-020-01313-0. [ Links ]
28. Mahmoud A, Abid F, Ezdini M, Lohdhiri ML, Ouanes I, Mesaaoud R. The contribution of simulation in training for funduscopic examination. La Tunisie Med. 2021;99(12):1T141-7. [ Links ]
29. Tso HL, Young J, Yung CW. comparing eyesi virtual reality simulator and traditional teaching methods for direct ophthalmoscopy: students’ perspectives at Indiana University School of Medicine. J Acad Ophthalmol . 2021 Jan;13(01):66-72. doi: http://dx.doi.org/10.1055/s-0041-1726349. [ Links ]
30. Wu C, Luo M, Liu Y, Dai R, Zhang M, Zhong Y, et al. Application of a 3D-printed eye model for teaching direct ophthalmoscopy to undergraduates. Graefe’s Arch Clin Exp Ophthalmol . 2022 Jan 17;260(7):2361-8. doi: http://dx.doi.org/10.1007/s00417-021-05538-w. [ Links ]
31. Howell GL, Chávez G, McCannel CA, Quiros PA, Al-Hashimi S, Yu F, et al. Prospective, randomized trial comparing simulator-based versus traditional teaching of direct ophthalmoscopy for medical students. Am J Ophthalmol . 2022 June;238:187-96. doi: http://dx.doi.org/10.1016/j.ajo.2021.11.016. [ Links ]
32. Belyea DA, Brown SE, Rayyoub LZ. Influence of surgery simulator training on ophthalmology resident phacoemulsification performance. J Cataract Refract Surg. 2011;37(10):1756-61. doi: https://doi.org/10.1016/j.jcrs.2011.04.032. [ Links ]
33. Oliveira SN, Kempfer SS. Utilização da simulação no ensino da enfermagem: revisão integrativa Rev Min Enferm. 2020;18(2):487-95. doi: https://doi.org/10.1590/s0080-62342012000100028. [ Links ]
34. Dourado ASS, Gianella, TR. Ensino baseado em simulação na formação continuada de médicos: análise das percepções de alunos e professores de um Hospital do Rio de Janeiro. Rev Bras Educ Med . 2014;38(4):10-8. doi: https://doi.org/10.1590/S0100-55022014000400007. [ Links ]
35. Cazanti RF, Fontes CER, Petta BFV. Dispositivo com câmera para treinamento de intubação orotraqueal: possibilidade de ensino médico em período pandêmicoRev Bras Educ Med . 2023;47(3):3-8. doi: https://doi.org/10.1590/1981-5271v47.3-2022-0083. [ Links ]
36. Dias MLS, Kadosaki DJ, Sousa IS, David JPF, Caldas IVR, Chaves RO Simulador para o treinamento do reflexo vermelho em recém-nascidos. Rev Bras Educ Med . 2021:45(1):10-5. doi: https://doi.org/10.1590/1981-5271v45.1-20200156.ING. [ Links ]
37. Mantora S, Sandinha MT, Ajith A, Song A, Steel DHW. Smart phone ophthalmoscopy: a potential replacement for the direct ophthalmoscope. Eye. 2018 July 24;32(11):1766-71. doi: http://dx.doi.org/10.1038/s41433-018-0177-1. [ Links ]
38. Wu AR, Fouzdar-Jain S, Suh DW. Comparison study of funduscopic examination using a smartphone-based digital ophthalmoscope and the direct ophthalmoscope. J Pediatr Ophthalmol. 2018 May;55(3):201-6. doi: http://dx.doi.org/10.3928/01913913-20180220-01. [ Links ]
39. Kim Y, Chao DL. Comparison of smartphone ophthalmoscopy vs conventional direct ophthalmoscopy as a teaching tool for medical students: the COSMOS study. Clinical Ophthalmology. 2019 Feb;13:391-401. doi: http://dx.doi.org/10.2147/opth.s190922. [ Links ]
40. Shikino K, Suzuki S, Hirota Y, Kikukawa M, Ikusaka M. Effect of the iExaminer Teaching Method on Fundus Examination Skills. JAMA Network Open. 2019 Sept 20;2(9): e1911891. doi: http://dx.doi.org/10.1001/jamanetworkopen.2019.11891. [ Links ]
41. Curtis R, Xu M, Liu D, Kwok J, Hopman W, Irrcher I, et al. Smartphone compatible versus conventional ophthalmoscope: a randomized crossover educational trial. J Acad Ophthalmol . 2021 July;13(02):270-6. doi: http://dx.doi.org/10.1055/s-0041-1736438. [ Links ]
42. Kohler J, Tran TM, Sun S, Montezuma SR. Teaching smartphone funduscopy with 20 Diopter lens in undergraduate medical education. Clinical Ophthalmology . 2021 May;15:2013-23. doi: http://dx.doi.org/10.2147/opth.s266123. [ Links ]
43. Ahmed Y, Pereira A, Rai AS, Leung VC, Ahmed A, Rai AS. Prospective evaluation of medical student accuracy conducting direct ophthalmoscopy with an unmodified iPhone X. Int Ophthalmol. 2022 July 23;42(12):3933-40. doi: http://dx.doi.org/10.1007/s10792-022-02377-4. [ Links ]
44. Qader AA, Er HM, Sow CF. The effectiveness of smartphone ophthalmoscope compared to direct ophthalmoscope as a teaching tool. The Asia Pacific Scholar. 2022;7(4): 22-34. doi: http://dx.doi.org/10.29060/taps.2022-7-4/oa2735. [ Links ]
45. Queiroz MS, de Carvalho JX, Bortoto SF, de Matos MR, das Graças Dias Cavalcante C, Andrade EAS et al. Diabetic retinopathy screening in urban primary care setting with a handheld smartphone-based retinal camera. Acta Diabetol. 2020;57(12):1493-99. doi: https://doi.org/10.1007/s00592-020-01585-7. [ Links ]
46. Corr RH. Fundoscopy in the smartphone age: current ophthalmoscopy methods in neurology. Arq Neuropsiquiatr. 2023;81(5):1-8. doi: https://doi.org/10.1055/s-0043-1763489. [ Links ]
47. Milani BY, Majdi M, Green W, Mehralian A, Moarefi M, Oh FS, et al. The use of peer optic nerve photographs for teaching direct ophthalmoscopy. Ophthalmology. 2013 Apr;120(4): 761-5. doi: http://dx.doi.org/10.1016/j.ophtha.2012.09.020. [ Links ]
48. Krohn J, Kjersem B, Høvding G. Matching fundus photographs of classmates. An informal competition to promote learning and practice of direct ophthalmoscopy among medical students. J Vis Commun Med. 2014 Apr 2;37(1-2):13-8. doi: http://dx.doi.org/10.3109/17453054.2014.884551. [ Links ]
49. Byrd JM, Longmire MR, Syme NP, Murray-Krezan C, Rose L. a pilot study on providing ophthalmic training to medical students while initiating a sustainable eye care effort for the underserved. JAMA Ophthalmol. 2014 Mar 1º;132(3):304-9. doi: http://dx.doi.org/10.1001/jamaophthalmol.2013.6671. [ Links ]
50. Lowe J, Cleland CR, Mgaya E, Furahini G, Gilbert CE, Burton MJ, et al. The arclight ophthalmoscope: a reliable low-cost alternative to the standard direct ophthalmoscope. J Ophthalmol. 2015:2015:743263 doi: 1155/2015/74363 Epub 2015 Sep 17 PMID: 2645.7197. PMCID: PMC 4589625 [ Links ]
51. Schulz C, Moore J, Hassan D, Tamsett E, Smith CF. Addressing the “forgotten art of fundoscopy”: evaluation of a novel teaching ophthalmoscope. Eye. 2015 Nov 13;30(3):375-84. doi: http://dx.doi.org/10.1038/eye.2015.238. [ Links ]
52. Lippa LM, Anderson CL. Assessment of durability of online and multisensory learning using an ophthalmology model. Ophthalmology . 2015 Oct;122(10):1960-6. doi: http://dx.doi.org/10.1016/j.ophtha.2015.06.027. [ Links ]
53. Yusuf I, Yang E, Knight K, Leaver L. Direct ophthalmoscopy: teaching in primary care. The Clinical Teacher [Internet]. 2015 May 15;13(3):235-7. doi: http://dx.doi.org/10.1111/tct.12354. [ Links ]
54. Kwok J, Liao W, Baxter S. Evaluation of an online peer fundus photograph matching program in teaching direct ophthalmoscopy to medical students. Can J Ophthalmol . 2017 Oct;52(5): 441-6. doi: http://dx.doi.org/10.1016/j.jcjo.2017.02.020. [ Links ]
55. Wilson AS, O’Connor J, Taylor L, Carruthers D. A 3D virtual reality ophthalmoscopy trainer. Clin Teach . 2017 Apr 12;14(6):427-31. doi: http://dx.doi.org/10.1111/tct.12646. [ Links ]
56. Bénard-Séguin É, Kwok J, Liao W, Baxter S. Use of a fundus photograph matching program in imparting proficiency in ophthalmoscopy. Can J Ophthalmol . 2018 Oct;53(5):480-5. doi: http://dx.doi.org/10.1016/j.jcjo.2017.11.022. [ Links ]
57. Dissanayake MM, Mathangasinghe Y, Weerakoon DN, Prasanni WDD. Videotape versus live demonstration in enhancing the technique and confidence of direct ophthalmoscopy in undergraduate medical education: a randomized controlled trial in a South Asian medical school. The Journal of the College of Ophthalmologists of Sri Lanka. 2017;23:25-30. [ Links ]
58. Boden KT, Rickmann A, Fries FN, Xanthopoulou K, Alnaggar D, Januschowski K, et al. Evaluierung eines VR-Simulators zum Erlernen der direkten Ophthalmoskopie in der studentischen Lehre. Der Ophthalmologe . 2019;117(1):44-9. doi: http://dx.doi.org/10.1007/s00347-019-0909-z. [ Links ]
59. Gilmour-White JA, Picton A, Blaikie A, Denniston AK, Blanch R, Coleman J, et al. Does access to a portable ophthalmoscope improve skill acquisition in direct ophthalmoscopy? A method comparison study in undergraduate medical education. BMC Med Educ . 2019 June 13;19(1):1-8. doi: http://dx.doi.org/10.1186/s12909-019-1644-5. [ Links ]
60. Lee JY, Gallo RA, Alabiad CR. Evaluating the effectiveness of small-group training in teaching medical students integral clinical eye examination skills. J Acad Ophthalmol . 2020 Jan;12(01):e79-86. doi: http://dx.doi.org/10.1055/s-0040-1712175. [ Links ]
61. Rose JS, Lalgudi S, Joshua RA, Paul J, Susanne MA, Phillips A, et al. A validated audio-visual educational module on examination skills in ophthalmology for undergraduate medical students in the Covid-19 season: an observational longitudinal study. Indian J Ophthalmol. 2021;69(2):400-405. doi: http://dx.doi.org/10.4103/ijo.ijo_2054_20. [ Links ]
62. Dunn HP, Kang CJ, Marks S, Witherow JL, Dunn SM, Healey PR, et al. Perceived usefulness and ease of use of fundoscopy by medical students: a randomised crossover trial of six technologies (eFOCUS 1). BMC Med Educ . 2021 Jan 8;21(1):41-9. doi: http://dx.doi.org/10.1186/s12909-020-02469-8. [ Links ]
63. Shikino K, Rosu CA, Yokokawa D, Suzuki S, Hirota Y, Nishiya K, et al. Flexible e-learning video approach to improve fundus examination skills for medical students: a mixed-methods study. BMC Med Educ . 2021 Aug 13;21(1):428. doi: http://dx.doi.org/10.1186/s12909-021-02857-8 [ Links ]
64. Vloka C, Wingrove P, Ong J, Koretz Z, Yadav S, Dmitriev A, et al. A novel approach to teaching fundoscopy using a virtual format. MedEdPORTAL. 2022 May 27;18:1-7. doi: http://dx.doi.org/10.15766/mep_2374-8265.11252. [ Links ]
65. Henick D, Labkovich M, Radell JE, Chopra N, Chadha N. Medical student attitudes toward the use of peer physical exam for learning fundoscopy. J Acad Ophthalmol . 2022 Jan;14(01): 60-69. doi: http://dx.doi.org/10.1055/s-0042-1743582. [ Links ]
Received: May 14, 2024; Accepted: January 24, 2025










 texto em
texto em